-

The Use Of Therapeutic Exercise And Manual Therapy For A Patient Following Simultaneous Bilateral Total Knee Arthroplasty: A Case Report
Allison Maynes
Osteoarthritis (OA) is the most common joint disorder in the United States (US) and is the most common cause for a total knee arthroplasty (TKA) surgery. Approximately 670,000 TKA surgeries are performed annually in the US and it is estimated that one third are bilateral TKAs (BTKA) due to bilateral OA. Simultaneously, BTKA procedures consist of replacing both knees consecutively,...Read More
-
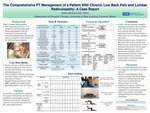
The Comprehensive PT Management Of A Patient With Chronic Low Back Pain And Lumbar Radiculopathy: A Case Report
Robin McGuire
Lumbar radiculopathy is pain originating from nerve root compression in the lumbar spine. Patient presentation is chronic, recurring low back pain with associated radiating pain and potential sensory, strength, or reflex deficits in the involved lower extremity. The purpose of this case report was to describe a comprehensive approach for a patient with chronic low back pain and lumbar radiculopathy...Read More
-

Developing Effective Online Training Tools For Maine Adaptive Sports And Recreation
Chelsea Paul, Emily Gall, Kristina Jamo, and Shannon Bergeland
Maine Adaptive Sports & Recreation (MASR) is an adaptive sporting program that relies on volunteers to instruct participants of varying abilities. In order to effectively instruct, volunteers should firmly understand the health condition their participant has. Previously, MASR lacked a formal curriculum to educate their volunteers. The aim of this research project was to create online learning modules & determine...Read More
-

Task-Oriented Training To Restore Independence In A Patient With Encephalitis In The Intensive Care Unit: A Case Report
Victoria Perez
Bacterial meningitis is a serious disease that causes acute inflammation of the meninges, the lining of the brain and spinal cord, which can result in significant morbidity and mortality. There are 15,000 to 25,000 cases in the US yearly and it is one of the top 10 causes of infection-related deaths worldwide. Bacterial meningitis is commonly complicated by encephalitis, inflammation...Read More
-

The Role Of Physical Therapy Interventions For An Elderly Patient Following Surgical Fixation Of A Fracture Of The Femoral Shaft: A Case Report
Ashley Push
In the U.S. approximately half of elderly white females will sustain an osteoporotic hip fracture. One year following surgery most elderly adults have not returned to their prior level of function. Evidence demonstrates the benefits of early weight bearing and mobility post-surgery to improve functional abilities. The purpose of this case report was to document this patient’s response to skilled...Read More
-
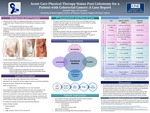
Acute Care Physical Therapy Status Post Colostomy For A Patient With Colorectal Cancer: A Case Report
Elizabeth Race
Colorectal cancer (CRC) is a malignancy that begins in the colon or rectum. In 2016 there were 724,690 men and 727,350 women living with a history of CRC, with an estimated 135,430 new cases in 2017. Treatment can include local radiation, systemic chemotherapy, and/or surgery to remove the tumor, which can result in the placement of a colostomy. A colostomy...Read More
-

The Use Of Manual Lumbar Traction And Therapeutic Exercise In The Treatment Of A Patient With Low Back Pain: A Case Report
Kyle Rasmussen
The prevalence of low back pain (LBP) has been increasing in the United States. Manual lumbar traction and therapeutic exercise are two common treatments by physical therapists (PT) for LBP, but there is limited research investigating the combined effects of these treatments on low back pain. The purpose of this case report was to investigate the combined effects of these...Read More
-

Vestibular Rehabilitation For A Geriatric Patient With Benign Paroxysmal Positional Vertigo Treatment Failure: A Case Report
Clare Roeder
Good balance requires integration of sensory information from three systems: vestibular, visual and somatosensory. The vestibular portion of the inner ear contains two types of sensory structures that respond to gravity and head movements: semicircular canals and otolith organs. Crystals of calcium carbonate (otoconia) reside in the otolith organs, but can become dislodged and migrate to the semicircular canals, causing...Read More
-

Strength And Balance Training For A 29-Year-Old Female Who Sustained A Multifocal Stroke: A Case Report
Britney Simonton and Kirsten Buchanan
Stroke is defined as a decrease in blood supply to the brain, and most often occurs in older adults. In the United States, approximately 795,000 people sustain a stroke annually. Risk factors for a stroke include high blood pressure, smoking, diabetes, and high cholesterol. Stroke is the leading cause of disability in the United States. Although research has shown that...Read More
-

Physical Therapy Management Of A Patient With A Lacunar Stroke And Multiple Comorbidities: A Case Report
Kevin Tachibana
Strokes are the fourth leading cause of death and the number one cause of long-term disability in the United States. A lacunar infarct is a type of ischemic stroke that occurs within the deepest structures of the brain when one of the small arteries gets blocked. Risk factors for a lacunar stroke include older age, high blood pressure, smoking, excessive...Read More
-
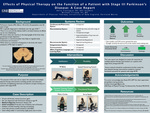
Physical Therapy On The Function Of A Patient With Stage III Parkinson’s Disease: A Case Report
Kelly Trancygier and Michaael Fillyaw
Parkinson’s disease (PD) affects 1.5% of the US population over 65 years of age. PD is typically diagnosed in individuals over the age of 60. There is no cure and the disease itself is not fatal, however, its effects can be very debilitating. PD occurs when the neurons in the basal ganglia of the brain stop producing enough dopamine. Dopamine...Read More
-

Functional Strengthening In A Patient With Chronic Stroke And Low Back Pain: A Case Report
Sofia Tzortzinis
In the U.S., the prevalence of stroke is approximately 795,000 annually and is the fifth most common cause of death. Stroke impairments include hemiplegia, sensory loss, dyspraxia, and hemianopsia. The chronic phase of stroke is defined as six months and beyond post-stroke. Nearly 85% of adults will experience low back pain (LBP) at some point in their life. Risk factors...Read More
-

The Physical Therapy Management Of A Patient With Chronic Shoulder Dislocations And Chronic Inflammatory Demyelinating Polyneuropathy: A Case Report
Lindsey Umapathy
Chronic shoulder dislocation is a severe disabling condition that can significantly decrease an individual’s quality of life, most often resulting after neglected acute dislocations, after surgery, or with the presence of unidirectional or multi-directional shoulder instability. Chronic Inflammatory Demyelinating Polyneuropathy (CIDP) is a neurological disorder characterized by progressive weakness and impaired sensory function in the legs and arms; it is...Read More
-

A Comprehensive PT Program Utilizing An AlterG Treadmill For A Patient With Lower Extremity Fractures And Charcot-Marie-Tooth Disease: A Case Report
Mark Whitsitt and Kirsten Buchanan
People with Charcot-Marie-Tooth (CMT) disease have a greater risk of falls and subsequent fractures due to lower extremity stiffness, muscle wasting, and balance impairments. Positive pressure treadmill systems, such as the AlterG®, are commonly utilized for orthopedic patients, as they allow for early mobility with decreased symptoms. Minimal research exists that has investigated use of the AlterG® in patients with...Read More
-
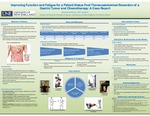
Improving Function And Fatigue For A Patient Status Post Thoracoabdominal Resection Of A Gastric Tumor And Chemotherapy: A Case Report
Michala Williams
A gastrointestinal stromal tumor (GIST), a type of stomach cancer, occurs when abnormal cells develop in the tissue of the gastrointestinal tract. Stomach cancer is a relatively rare carcinoma that is often not detected until later stages. The purpose of this case report was to document the physical therapy approach for a deconditioned patient due to resection of a malignant...Read More
-

Application Of Manual Therapy Utilizing Maitland Principles In The Rehabilitation Of A Patient Following Rotator Cuff Repair
Kehinde Aderibigbe and Brian T. Swanson
In the United States, more than 500,000 rotator cuff repairs and shoulder arthroscopies are performed annually. Following surgery, physical therapy (PT) often utilizes various manual therapy (MT) and therapeutic exercise (TE) interventions. Post-operatively, accessory joint mobilizations (AJM) help to prevent adhesions and may decrease excitability of central nociceptive pathways. However, there is no consensus about the most appropriate postoperative utilization...Read More
-

Physical Therapy Treatment Of A Patient With Chronic Low Back Pain And A Previous History Of A Substance Abuse Disorder: A Case Report
Marcus X. Alomar and Brian T. Swanson
The National Survey on Drug Use and Health (NSDUH) reported that an estimated 27 million people in the United States have reported use of an illicit drug within the past month. Low back pain continues to be a major cause of disability in the United States, with an estimated 70 percent of adults experiencing low back pain at some point...Read More
-

Combining Physical Therapy And Podiatry For A Patient With Plantar Fasciitis: A Case Report
Kathleen Barnes and Kirsten Buchanan
One million cases of plantar fasciitis (PF) are reported annually in the United States. Studies have separately investigated the effectiveness of physical therapy (PT) interventions as well as steroid injections from podiatry – but not in conjunction with each other. There is a lack of research investigating an interdisciplinary approach utilizing PT and podiatry for PF. This case report investigated...Read More
-
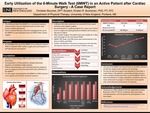
Early Utilization Of The 6-Minute Walk Test (6MWT) In An Active Patient After Cardiac Surgery - A Case Report
Christian Boucher and Kirsten Buchanan
Coronary artery disease affects more than 13 million Americans. A sub-population of these patients, despite exercising regularly, can develop cardiac disease. The 6-Minute Walk Test (6MWT) is a functional outcome measure that is easy to implement and has been used across multiple populations. There is limited literature that has investigated the use of the 6MWT on post-operative day one (POD1)...Read More
-
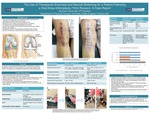
The Use Of Therapeutic Exercises And Manual Stretching For A Patient Following A Total Knee Arthroplasty (TKA) Revision: A Case Report
Nicholas Cebula
Total knee arthroplasty (TKA) is an orthopedic surgery involving the total replacement of compartments of the knee joint. Osteoarthritis (OA) is the most common reason for TKA. Risk factors for OA include: obesity, sports-related injuries, and genetics. The artificial knee joint typically lasts between 15-20 years; early failures may occur due to loosening of artificial components, infection, fractures, and instability....Read More
-

The Use of Manual Therapy In The Treatment Of A Patient With Chronic Low Back Pain And Sciatica: A Case Report
Elia N. Darazi
Low back pain (LBP) is the second most common cause of disability in adults with total costs estimated to be between $100 and $200 billion annually on the US economy. The prevalence of chronic LBP rose significantly over a 14-year interval (1992 to 2006), from 3.9% to 10.2%. Treatment of LBP may be conservative or surgical, with conservative being the...Read More
-

Physical Therapy Intervention For A Patient With Temporomandibular Joint Dysfunction Caused By Two Traumatic Events: A Case Study
Elyse Detweiler
Temporomandibular disorders (TMD) are a collection of pathoanatomical dysfunctions of the temporomandibular joint (TMJ) and are associated with a variety of symptoms throughout the head and neck. There is a severe lack of supportive evidence for physical therapy management used in the conservative and/or post-surgical treatment of TMD. The dental profession provides much of the current literature on TMD but...Read More
-
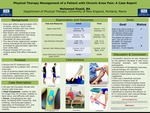
Physical Therapy Management Of A Patient With Chronic Knee Pain: A Case Report
Mohamed Elsaid
Knee pain affects approximately 25% of adults, and as a result limits functional mobility and may induce participation restrictions. Risk factors may contribute to knee pain, with osteoarthritis (OA) being the most prevalent cause in individuals 50 years and older. The rate of knee replacement surgery among individuals 65 and older has increased by approximately eight fold from 1979-2002. Physical...Read More
-

Physical Therapy Management Of A Patient After Hemorrhagic Stroke Using A Task-Oriented Approach In A Skilled Nursing Facility: A Case Report
Kaela Fischer
Stroke is the leading cause of long term disability in the U.S.; nearly 800,000 Americans have a stroke each year. Subarachnoid hemorrhagic stroke occurs when one of the blood vessels in the brain bursts causing a release of blood which increases intracranial pressure. There is a lack of rehabilitation research in the skilled nursing setting for hemorrhagic stroke. The purpose...Read More
-

Physical Therapy Management Of A Patient With Chronic Brainstem Stroke Syndrome To Improve Functional Mobility: A Case Report
Kelley Flahaven
Strokes are a leading cause of disability, and the fifth leading cause of death in the U.S. Brainstem strokes are much less common and have a higher mortality rate than cortical strokes. Brainstem strokes can lead to physical impairments including gaze palsies, quadriplegia, ataxia, or cranial nerve deficits, which affect balance and safety, decreasing independence. Repetitive task gait training has...Read More
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.


