-

Treatment Of A Patient With Thoracolumbar Scoliosis Utilizing A Regional Interdependence Approach Including Components Of The Schroth Method: A Case Report
Samantha Fisk
Spinal deformity is a challenging spinal disorder in adults. A scoliotic curve of >10 degrees exists in up to 12% of the population. There is little evidence regarding indications for physical therapy treatment in elderly individuals with adult scoliosis. Current study results favor surgical intervention, but not all elderly individuals are surgical candidates. While surgery is the definitive measure, there...Read More
-

Use Of Therapeutic Exercise, Functional Endurance And Gait Re-Training In A Deconditioned Patient With Acute Respiratory Failure: A Case Report
Ellen Forslund
The human body requires oxygen-rich blood in order to work efficiently. During respiration, air passes from the nose and mouth and into the alveoli of the lungs. When air reaches the alveoli, oxygen passes into the capillaries as carbon dioxide moves out of the capillaries, otherwise known as gas exchange. Respiratory failure may occur when there is a lack of...Read More
-

Neuromuscular Strengthening Exercises Following ACL And Meniscal Repair In A 15 Year Old Female Athlete With Generalized Knee Laxity: A Case Report
Alyssa Gardner and Kirsten Buchanan
Adolescent females are 4-6 times more likely to sustain a non-contact anterior cruciate ligament (ACL) injury compared to their male counterparts. Generalized knee laxity decreases dynamic knee stability and significantly increases the odds of an ACL injury 5-fold. It is crucial to return the surgically repaired knee to its former function. However, it is just as vital to direct attention...Read More
-

The Use Of Manual Therapy And Strengthening Exercises To Improve Plantarflexion Strength And Mobility Following Achilles Tendon Repair: A Case Report
Jason Glikman
An Achilles tendon rupture is classified as ‘chronic’ or ‘neglected’ if it has been untreated for four or more weeks. PT management for all Achilles ruptures is to gain Plantarflexion (PF) strength, ankle ROM, and decrease scar tissue. Neglected ruptures increase scar tissue formation, causing delay in regaining functional strength and mobility. Decreased strength and mobility can lead to gait...Read More
-

Using The Selective Functional Movement Assessment And Regional Interdependence Theory To Guide Treatment Of An Athlete With Back Pain: A Case Report
Gabriella Goshtigian
Incidence of low back pain (LBP) is as high as 36% among adolescents and even more prevalent in those who play sports. The majority of these cases lack an underlying diagnosis and are classified as non-specific LBP. Previous injury and longer durations of pain consistently emerge as prognostic factors in musculoskeletal pain. This affects movement patterns which then continue to...Read More
-

The Use Of Aquatic Therapy In Rehabilitation For A Patient Following Complicated Reverse Total Shoulder Arthroplasty: A Case Report
Alyssa Grigware
According to the Aquatic Physical Therapy Section of the American Physical Therapy Association, aquatic physical therapy is the evidence-based and skilled practice of physical therapy in an aquatic environment by a physical therapist, and includes interventions designed to improve or maintain: function, aerobic capacity/endurance conditioning, balance, coordination and agility, body mechanics and postural stabilization, flexibility, gait and locomotion, relaxation, muscle...Read More
-

Neuromuscular Electrical Stimulation And Quadriceps Strength Following Patellar Fracture And Open Reduction Internal Fixation Surgery: A Case Report
Chelsea Hussey
Patellar fractures account for approximately 1% of all fractures and are most common in people who are 20 to 50 years old. Comminuted patellar fractures occur when the bone shatters into three or more pieces and is usually caused by a direct blow to the knee. Open reduction internal fixation (ORIF) surgery is typically needed if the bone is broken...Read More
-

Functional Skill Training And Group Therapy Treatment Following A Total Hip Arthroplasty In The Acute Care Setting: A Case Report
Heidi Johnson
Osteoarthritis (OA) is a very common degenerative condition, often developed during middle and older ages, especially in those with more active lifestyles. Although OA can occur in any joint throughout the body, it most often develops in weight-bearing joints, such as the hip. In 2011 more than 28 million people in the United States were estimated to have OA. OA...Read More
-

Hip Muscle Strengthening And Balance For A Patient With Bipolar Disorder Following Hip Fracture: A Case Report
Allison Kaplan
Hip fractures result in more than 258,000 hospital admissions annually for those aged 65 and older. Mortality rate following hip fracture is 10-20%. Among survivors, half will have longstanding disability, only 1/3 will return home, and 19-27% will remain in long term care. Six percent will experience a second fracture within four years. Cost for treatment for hip fractures in...Read More
-

The Role Of Physical Therapy In The Treatment And Discharge Of An Elderly Homeless Patient With Fractures Of The T12-L1 Vertebrae: A Case Report
Matthew Kraft
More than 600,000 are homeless in the USA. Homeless people have higher rates of premature mortality than the rest of the population, especially from unintentional injuries, and have an increased prevalence of mental disorders. Hospitals often encounter difficulty with discharge when homeless patients are medically stable enough to be transferred to a lower level of care. Hospitals risk potential legal...Read More
-

Restoring Functional Mobility In A Patient With Delayed Onset Of Physical Rehabilitation Following A Hemorrhagic Stroke: A Case Report
Bettie Kruger and G. Noel Squires
Typical rehabilitation post-stroke is initiated as soon as the patient is medically stable. The most dramatic neurological recovery occurs within the first three to six months following medical stabilization. It has been suggested in the literature that early and frequent out of bed activity within the first 24 hours following stroke onset will enhance motor recovery. The patient in this...Read More
-

Strength And Balance Exercises To Improve Functional Outcomes And Mobility For A Patient With Parkinson’s Disease And Co-morbidities: A Case Report
Nicholas LaSarso
Parkinson’s disease is the second most common age-related neurodegenerative disorder after Alzheimer’s disease. Cardinal features include rigidity, bradykinesia, tremor and postural instability. There is a lack of literature pertaining to the physical therapy management of patients with Parkinson’s Disease and other co-morbidities. The purpose of this case report was to illustrate the physical therapy management of a patient with Parkinson’s...Read More
-

Functional Mobility Management Of A Patient With Adult-Onset Hereditary Proximal Motor Neuropathy Following A Tibial Fracture: A Case Report
Timothy Lira and Amy J. Litterini
This patient was clinically appealing and complex because of the combination of an acute fracture due to an injurious fall and significant past medical history (PMH) of both the rare condition of adult-onset hereditary proximal motor neuropathy (AHPMN) and congestive heart failure (CHF). The chronic co-morbidities created the need for an innovative approach to treatment sequencing to potentially mitigate the...Read More
-
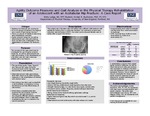
Agility Outcome Measures And Gait Analysis In The Physical Therapy Rehabilitation Of An Adolescent With An Acetabular Hip Fracture: A Case Report
Emily Lodge and Kirsten Buchanan
Pediatric hip fractures are uncommon. 85 to 90 percent of pediatric hip fracture are a result of high-energy trauma. There is a paucity of literature describing best rehabilitation practices. Agility outcome measures, as well as observational and video gait analysis have not been fully investigated in the rehabilitation of pediatric hip fractures. The purpose of this case report was to...Read More
-

Use Of Manual Therapy And Sport Specific Re-training In An Adolescent Elite Sprinter With Bilateral Pedicle Stress Fractures: A Case Report
Erika Lopez
Bilateral pedicle stress fractures are extremely rare, with few cases reported in the literature. The pedicle is known to be the second weakest point of the vertebra, has a short moment arm from the vertebral body, and can resist a large amount of cyclic shear forces. The main causes of lumbar pedicle stress fractures are shear stress and twisting stressors,...Read More
-

The Use Of Postural Reeducation And Strengthening Exercises In The Reversal Of Functional Scoliosis: A Case Report
Cory Marcoux
Non-structural scoliosis: abnormal spinal curvatures that have sufficient mobility, and can therefore resolve with postural change. There is a multitude of research regarding structural and idiopathic scoliosis, but very minimal literature about non-structural (functional) scoliosis and more importantly, how to treat it. The purpose of this case report was to examine the use of stretching, strengthening, and postural reeducation for...Read More
-
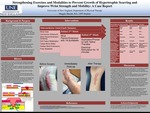
Strengthening Exercises And Modalities To Prevent Growth Of Hypertrophic Scarring And Improve Wrist Strength And Mobility: A Case Report
Maggie Masiak
There is no gold standard for evaluation, treatment, and prevention of keloids. Keloids are elevated fibrous scars that extend beyond the original borders of the wound, they do not regress and they tend to reoccur even after surgical excision. Individuals younger than 30, with elevated hormone levels and darker skin tend to be at higher risks for keloids. The most...Read More
-

Vestibular Rehabilitation For A 17-Year Old Female With Post-Concussion Symptoms: A Case Report
Elizabeth Mosley
Post-concussion syndrome is defined as a group of symptoms occurring after a traumatic brain injury (TBI) that can last weeks, months, or years. The diagnosis of post-concussion syndrome is not well agreed upon, but does include at least three of the following symptoms: headache, dizziness, fatigue, irritability, insomnia, concentration or memory difficulty, and intolerance of stress or emotion. The Centers...Read More
-

The Clinical Decision Making And Outcomes Of A Patient With C7, C8 Radiculopathy And Contralateral Upper Quarter Lateral Epicondylitis: A Case Report
Courtney Naimi
Preliminary diagnosis and management strategies exist for both cervical radiculopathy (CR) and lateral epicondylis, however little literature exists describing the clinical decision making and management in the presence of both conditons simultaneously. Management of (CR) (right side) can include neural mobilizations, manual therapy, and exercises. Management of lateral epicondylis (left side) can include eccentric tendinopathy management and manual therapy. The...Read More
-

Conservative Physical Therapy Protocol After Subacromial Decompression And Labral Debridement In A Young Former Competitive Gymnast: A Case Report
Sara Nichols and Kirsten Buchanan
Subacromial impingement syndrome is a musculoskeletal condition characterized by shoulder pain and altered glenohumeral kinematics. Conservative treatment can include physical therapy and corticosteroid injections. Surgical option includes subacromial decompression (SAD). Most patients who undergo SAD are approximately 50-60 years old. There is little to no evidence regarding rehabilitation of young, healthy individuals following SAD. The purpose of this case report...Read More
-

Functional Training To Reduce Fall Risk In A Patient Following Cancer Treatment: A Case Report
Kristin O'Kelly
The National Cancer Institute reports that 39.6% of men and women will be diagnosed with some form of cancer during their lifetime. Studies have demonstrated that over half of cancer survivors age 55 and over have fallen in the past year, possibly as a result of treatment and subsequent muscle weakness, difficulty with balance, and impaired walking. Multiple studies have...Read More
-

Application Of A Balance Training Program In A Patient With Charcot Marie Tooth Disease: A Case Report
Eduardo Pena
Charcot Marie Tooth Disease (CMT) is the most common progressive inherited neurological disease. Proteins in the myelin sheath of both motor and sensory nerves become damaged, resulting in muscle atrophy and reduced sensation. Patients experience difficulty with gait, balance, and independence with ADLs. The RUSK Modified Romberg Program (MRP) is a balance program used for patients with neurological pathologies. There...Read More
-

A Task Oriented Approach For A Patient With Chronic Effects Of Stroke: A Case Report
Sarah Richardson and Amy J. Litterini
Stroke is the leading cause of serious long-term disability for American adults. Most stroke survivors receive physical therapy (PT) and task-oriented rehabilitation is one novel approach. This technique, which shifts the focus from the impairment level to activity level, is known to benefit stroke survivors. However, the benefits for long-term survivors of stroke are not yet well established. PT professionals...Read More
-

Multimodal Physical Therapy Management Of A Patient With Unilateral Neglect Post-Stroke In An Outpatient Setting: A Case Report
Meghan Riley
A common behavioral syndrome of stroke is unilateral neglect (ULN) which is defined as the failure to report, respond, or orient to stimuli presented contralateral to the brain lesion. ULN has a negative influence on functional recovery and is associated with a poor functional outcome following a stroke, therefore several rehabilitative approaches have been proposed and implemented to decrease neglect...Read More
-

Use Of Complete Decongestive Therapy And A Task-Oriented Approach In Treating Secondary Lymphedema And Improving Ambulation In A Patient Following A Stroke: A Case Report
Snezhana Rudakova
Every year, approximately 795,000 people in the United States experience a new or recurrent stroke. More than 30% of the survivors cannot walk independently six months following a stroke. Of those who are able to walk independently, only a small proportion can walk with sufficient speed and endurance to be able to function within the community. Paralysis of the extremities...Read More
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.


