-

Physical Therapy Outcomes In A 28 Year Old Male With A Femoral Neck Fracture Using Aquatic And Land-Based Therapeutic Exercise: A Case Study
Daniel Johnson
Background: Hip fractures occur in approximately 341,000 persons each year in the U.S. Hip fractures at a young age are uncommon and are usually the result of a high-velocity injury or, rarely, secondary to bone pathology. Morbidity associated with an inability to return to a pre-fracture level of mobility often results in a loss of independence, reduction in quality of...Read More
-

The Effects Of Robot-Assisted Gait Training And Task-Specific Training On ADL Function And Mobility For A Patient After A Stroke: A Case Report
Maegen Johnson
Background: Stroke is the fourth leading cause of death and the leading cause of long term disability in the United States. Repetitive task-specific training has been shown to be favorable in stroke rehabilitation. Robot-assisted gait training (RAGT) incorporates gait training and repetitive task-specific training. RAGT has been shown to increase the likeliness of independent walking ability in patients who have...Read More
-

The Role Of An International Cross Cultural Interprofessional Healthcare Immersion Program In Doctor Of Physical Therapy Education: An Educational Case Report
Jayme Keith
Purpose: The purpose of this educational case report is to describe an interprofessional international cross-cultural immersion healthcare program and to discuss the role of this program in the development of Doctor of Physical Therapy (DPT) students’ cultural competence, interprofessionalism, and social responsibility. Description: The Ghana Cross Cultural Health Immersion (GCCHI) program provides annual primary health care services and education in...Read More
-

Physical Therapy Management Of A Patient With A Transtibial Amputation Using An Over-Ground Body Weight Support System: A Case Report
Elizabeth Kelly
Background: Peripheral Arterial Disease (PAD): Narrowing of the vessels secondary to atherosclerotic plaque buildup, results in ischemia to extremities which can lead to intermittent claudication, decreased distal pulses, impaired healing. Lower Extremity Amputation: 54% of amputations in the USA are due to PAD, either alone or in conjunction with diabetes (Kalapatapau V. et al), transtibial and transfemoral most common, best...Read More
-

Outpatient Physical Therapy Following Surgical Repair of a Left Patellar Tendon Rupture: A Case Report
Michael Kilgas
Patellar tendon tears often occur in patients less than 40 years old with forced flexion of the knee. Surgical repair of the tendon is most commonly the treatment following a tear; additionally, performing surgery to repair the tendon in a timely fashion is an important prognostic factor. The purpose of this case report is to outline the deficits following surgical...Read More
-

Physical Therapy Management Of A Patient With Guillain-Barre Syndrome During and After Pregnancy: A Case Report
Sarah Kou
Background: Guillain Barre Syndrome (GBS) is a disorder in which the body’s immune system attacks part of the peripheral nervous system. The cause of GBS is still unknown, with suspicions of viral or bacterial infection preceding diagnosis. It can affect people of all ages, gender, or ethnic background, with equal incidence rates in both men and women. The incidence rate...Read More
-
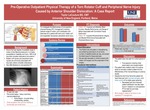
Pre-Operative Outpatient Physical Therapy Of A Torn Rotator Cuff And Peripheral Nerve Injury Caused By Anterior Shoulder Dislocation: A Case Report
Taylor LaCouture
Background: Due to the high degree of available range of motion of the Glenohumeral joint, it is highly susceptible to instability and injury. 98% of all traumatic shoulder dislocations are anterior. Rotator cuff injuries and peripheral nerve injuries are commonly associated with traumatic anterior shoulder dislocations. Very little literature exists on pre-operative PT. Purpose: To investigate the effectiveness of pre-operative...Read More
-

Physical Therapy Management Of A Patient After A Subacromial Decompression with Acromioplasty And Bursectomy: A Case Report
Brianne Landholt
Background: Subacromial impingement results from repetitive trauma to structures underneath the subacromial arch which can lead to: A decrease in the subacromial space, impingement of the soft tissue, a decrease in functional abilities. Conservative treatment can include: Physical therapy, nonsteroidal anti-inflammatory drugs (NSAIDS), corticosteriod injections, surgical option includes a subacromial decompression (SAD). There is conflicting evidence on the benefits of...Read More
-

Physical Therapy Management Of A Manual Laborer With Chronic Rotator Cuff Tendinopathy: A Case Report
Samuel Lasher
Background: Tendinopathy is characterized by tendon thickening, localized pain and chronic degeneration reflective of failed healing. 38% of manual laborers who participate in daily moderate to heavy lifting will experience Rotator Cuff Tendinopathy(RCT). There is a lack of research investigating the PT management of manual laborers who have RCT, but must continue to participate in harmful activities to fulfill occupational...Read More
-

The Physical Therapy Management Of A Patient With Adverse Mechanical Tension Including The Use Of Neural Gliders And Tensioners: A Case Report
Brent Manley
Background: Adverse mechanical tension on one’s nervous system can impair a nerves ability to mobilize in relation to its interfacing tissues and lead to sensations of pain, paresthesia and numbness. Common physical therapy intervention includes sliding and tensioning of the irritated nerve and managing the tissues surrounding it. Purpose: The purposes of this case report were to (1) provide overview...Read More
-

Balance And Functional Skill Training For A Patient With Cognitive Dysfunction And Impaired Safety Awareness: A Case Report
Cameron McCombs
Background: With advances in medicine, there are increasing numbers of people living who have had a stroke. One of the major factors that can limit improvement is cognitive dysfunction. Cognitive rehabilitation in conjunction with large amounts of repetition can result in lasting neuronal changes. Purpose: The purpose of this case study is to describe the decision making process for physical...Read More
-

Instrument Assisted Soft Tissue Mobilization and Conservative Management Of Shoulder Pain In An Elderly Male: A Case Report
Dana McCoy
Background: Shoulder pain is a frequent complaint among the elderly population, numerous etiologies cause shoulder joint pain such as osteoarthritis, adhesive capsulitis, and rotator cuff disease (impingement, tendonitis, and cuff tear). A conservative treatment for shoulder pathology is Augmented Soft Tissue Mobilization (ASTM) that uses specifically designed sold instruments to perform manual therapy. Sound Assisted Soft Tissue Mobilization (SASTM®) is...Read More
-

Outpatient Interventions For Femoral Acetabular Impingement Complicated By Hip Osteoarthritis, Labral Tear And L5 Sacralization: A Case Report
Brianna Palmer
Background: Femoral Acetabular Impingement (FAI) is a known cause of hip pain in adolescents and young adults produced by altered hip joint mechanics. Types of FAI include Cam deformity, Pincer deformity or a combination. Abnormal abutment of the femoral head on the acetabular rim, especially during hip flexion and internal rotation (IR) causes a sharp, pinching pain in the groin...Read More
-

Physical Therapy Management Of An In-Patient After Total Knee Arthroplasty: A Case Report
Jareth Pamer
Background: Increasing prevalence of knee OA and TKA; according to the American Academy of Orthopedic Surgeons, there will have been a half a million TKA procedures performed by 2030. Purpose: The purpose of this case report is to describe the physical therapy management of an in-patient status post total knee arthroplasty.
... Read More
-

Test-Retest Reliability And Minimal Detectable Change Of The Modified Fresno Test Of Evidence Based Practice In DPT Students
Erin Pike and Lisa Gerhardt
Poster presenting a research study whose purpose was to determine the test-retest reliability and MDC of the MFT in first, second, and third year DPT students, and to compare the mean total score of the MFT among the three student groups. Using a simple random sample, 21 students were recruited from each of the three UNE DPT classes. The participants...Read More
-

Acute Care PT Management Of A Patient Following A Total Knee Arthroplasty With Partial Weight Bear Orders Secondary To Bone Cyst In The Femur: A Case Report
John Quinn
Background: Total Knee Arthroplasy (TKA): OA is the most common joint disorder in the US. A TKA is a surgical procedure aimed to relieve signs and symptoms of severe osteoarthritis. Acute care following a TKA includes: Swelling management, increasing range of motion, enhancing muscle control and strength in the involved lower extremity, maximizing patient’s mobility with the goal of functional...Read More
-

The Pediatric PT Management Of A Survivor Of Cancer: A Case Report
Kaylene Samuels
Cancer in the cerebellum in a pediatric population is rare. The cerebellum is responsible for: coordination of ongoing movements, postural control, visual gaze, performing smooth purposeful movements. There is limited evidence investigating the physical therapy management of pediatric survivors of cancer, more specifically, in cerebellum brain tumors. The purpose of this case report was to investigate the PT management of...Read More
-

Outpatient Physical Therapy Following Surgical Debridement Of Osteochondritis Dissecans Of The Talar Dome: A Case Report
Angela Serrani
Background: Osteochondritis Dissecans (OCD): Alteration of subchondral bone with disruption of the adjacent articular cartilage; cause unknown, hypotheses include repetitive trauma and or non-traumatic disruption of subchondral blood supply; suspected chondral injury with up to 50% of ankle instability episodes. Treatment Options: Goals: relieve symptoms and improve function; non-surgical: rest, immobilization, NSAIDS; surgical: excision of lesion, excision with cutterage and/or...Read More
-

The Use Of An Orthotic Garment System On A Pediatric Patient With Mitochondrial Disease Complex 1+3: A Case Report
Stephanie Sheehan
Background: Mitochondrial Disease (MD) is a progressive and debilitating disease that is characterized by a loss of efficiency in the electron transport chain and reductions in the synthesis of high energy molecules such as ATP. Orthotic garment systems also referred to as “TheraTogs®”, have been designed to act as a continuous somatosensory guide for proper functional alignment. Theratogs have been...Read More
-

Improving Functional Independence With Rehabilitation Following A Metastatic Melanoma Brain Tumor Resection: A Case Report
Benjamin Sherr
History: A 67 year-old male with a one year history of melanoma complained of headaches 1-2 weeks prior to admission to an acute care hospital with left sided hemiplegia and dysarthria. A head CT scan revealed an intracerebral hematoma and a lesion suspicious for metastasis within the right parietal lobe. A right parietal craniotomy, evacuation of the hematoma and resection...Read More
-

Describing Regional Interdependence For A Patient With Lateral Epicondylalgia Managed With Postural Training And Iontophoresis: A Case Report
Matthew Starkey
Background: Lateral epicondylalgia describes a condition where pain and tenderness are present in the wrist extensors, most commonly from repetitive motion activities. Current research suggests the cause is attributed to tissue degeneration due to repetitive stress to the wrist extensors. A concept known as regional interdependence may also influence lateral epicondylalgia. Regional interdependence describes a condition where impairments are present...Read More
-

Outpatient Physical Therapy Management of a Breast Cancer Survivor Following Kyphoplasty with a Complex Medical History
Molly Thornton
Background and Purpose: There are over 3 million breast cancer survivors in the U.S. Cancer and its treatment can cause a wide variety of long-term physical and psychological problems. The physical therapist’s role is not well defined for this population. The purpose of this case report is to describe the outpatient physical therapy management for a patient with a history...Read More
-

Physical Therapy Management For A Patient With Low Back Pain Utilizing Medical Exercise Therapy
George Tsakos
Background: Low back pain (LBP) is one of the most common and costly musculoskeletal diagnosis in America. Approximately 50% of individuals with LBP have recurrent episodes by 1 year, 60% by 2 years and 70% by 5 years. Multiple studies have been inclusive determining a gold standard for cost effective long term outcomes. MET therapy focuses on early functional activity...Read More
-

Functional Mobility And Gait Training During Inpatient Rehabilitation Following Middle Cerebral Artery Stroke: A Case Report
Emily Wallingford
Mortality from stroke is the 4th leading cause of death in the US, and is a leading cause of long-term severe disability among adults. Incidences of disabilities include: hemiparesis, unable to walk without assistance, dependent in ADLs, aphasia, and depression. Stroke survivors represent the largest group admitted to rehabilitation hospitals and approximately 1 in 4 patients with stroke are placed...Read More
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.


