-

Restoring Functional Mobility Following A Ruptured Abdominal Aortic Aneurysm: A Case Report
Grace Laughlin
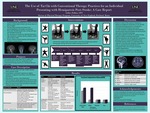
An abdominal aortic aneurysm (AAA) is a dilation of the abdominal aortic artery greater than three centimeters involving all layers of the vessel wall. There are two surgical options for treatment of AAA: open repair and endovascular aneurysm repair (EVAR). An endoleak is a complication following EVAR when blood leaks into the aneurysm sac. A type III endoleak occurs when...Read More
-
Tissue Plasminogen Activator Effects On Stroke And Physical Therapy Outcomes In Acute Care: A Case Report
Lindsey Leboeuf
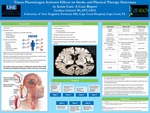
An ischemic stroke occurs when blood flow to an area of the brain is restricted by a blood clot. Symptoms include: Numbness or weakness on one side of the body, facial droop, trouble speaking, and trouble walking. Patients can also display decreased balance, ataxia, flaccidity, spasticity, inattention or neglect, and visual changes. Patients who can identify these symptoms within 3...Read More
-

Inpatient Rehabilitation For A Cancer Survivor Following A Lumbar Spinal Fusion Secondary To A Pathological Fracture: A Case Report
Nicole Marczak and Amy J. Litterini
Pathologic fractures are considered a skeletal-related event of bone metastasis. Bone metastases indicate a shorter prognosis with the survival rate varying from 6-53 months, depending on the primary type of cancer. Indications for surgery include spinal instability, vertebral collapse with or without neurologic deficit and intolerable pain that is not responsive to conservative treatment. Palliative physical therapy (PT) is provided...Read More
-
Balance And Strength Interventions For An Individual Post Left Sided MCA CVA: A Case Report
Annie McKenzie
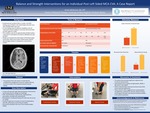
Cerebrovascular accident (CVA), or stroke, is the fifth leading cause of death in the United States (US) with more than 140,000 deaths each year. It is the leading cause of long-term disability in the US, reducing functional mobility in more than half of all stroke survivors ages 65 or older. This condition costs the US approximately 34 billion dollars a...Read More
-

A Hip Strengthening Protocol For A Patient Following Achilles Repair: A Case Report
Matthew Morris
The Achilles tendon is the most frequently ruptured tendon in the body and rupture most commonly occurs in men ages 30-50. Operative repair has more complications, but lower re-rupture rate, than non-operative management. Early weight-bearing after surgery has been shown to be beneficial. Hip weakness has been associated with lower extremity conditions such as gait deviations, ankle sprains, and knee...Read More
-

Outpatient Physical Therapy Management Of A Patient Following A Severe Left Middle Cerebral Artery Infarction: A Case Report
Ryan Parnell
A cerebral vascular infarction (CVI) is a loss of blood flow to an area of the brain, which results in cell damage and/or death. The most common occluded artery is the middle cerebral artery (MCA). The incidence of falls within one year following a CVI can be as high as 42-60%. CVIs are a leading cause of long-term disability in...Read More
-
Combining A Comprehensive Physical Therapy Program And Electroshock Therapy For A Patient With Plantar Fasciitis: A Case Report
Kathryn Piersiak
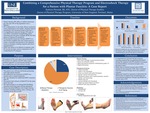
Plantar fasciitis (PF) affects 2 million Americans per year and 10% of the population over a lifetime. PF is inflammation to the thick, fibrous connective tissue originating on the medial calcaneal tubercle extending to the metatarsal heads of the foot. A comprehensive physical therapy (PT) plan of care (POC) of proximal strengthening, distal stretching and soft tissue massage (STM) has...Read More
-

Incline Treadmill Training For A Crush Ankle Injury With An Open Wound: A Case Report
Anna Prokity
Within the industrial workplace, soft tissue injuries to the ankle are common. The ankle is the second most commonly injured region in the body. Past research has shown that average time away from work was 2.5 weeks for a lateral ankle sprain, with 90% of individuals having full return to work at six weeks. Therapeutic activities are part of a...Read More
-

Using Video And Mobile Applications To Manage Distress Following Acute COPD Exacerbation With Respiratory Failure: A Case Report
Linda Rose Shober
Chronic lower respiratory diseases, mainly chronic obstructive pulmonary disorder (COPD), represent a significant economic burden to the healthcare system and are among the top three leading causes of death in the United States. An acute exacerbation of chronic pulmonary disorder (AECOPD) is a worsening of the respiratory symptoms associated with COPD including dyspnea, increased sputum production, cough, and airway obstruction....Read More
-

Home Health Physical Therapy For A 90-Year-Old Patient Following Transient Ischemic Attack: A Case Report
Kendra Stephens
Transient ischemic attack (TIA) is an episode of focal brain dysfunction that is temporary (<24 >hrs.) and is due to a dysfunction of an arterial territory of the brain. Its most common symptoms include facial droop, arm weakness, and speech difficulty. An estimated 200,000 to 500,000 people per year experience a TIA in the U.S. After having TIA, 1/3 of...Read More
-

Treatment Of A Work-Related Superior Glenoid Labral Repair: A Case Report
Alexandra Touri
A superior glenoid labrum tear is a common injury in the shoulder. The highest incidences of superior labrum tear from anterior to posterior (SLAP) lesions occur in individuals from 20-29 years old and 40-49 years old. Common signs and symptoms include: instability in the joint, shoulder dislocations, pain with overhead activities, decreased range of motion, and loss of strength. SLAP...Read More
-

Joint Stability And Proprioception Training To Reduce Chronic Pain For A Female Patient With Hypermobile Ehlers-Danlos Syndrome: A Case Report
Ashley Tullo
Ehlers-Danlos Syndrome (EDS) is a heritable connective tissue disorder with many subtypes. Hypermobile EDS (hEDS), the most common subtype, is characterized by generalized joint hypermobility, musculoskeletal impairments, systemic involvement, and a familial history of EDS. Due to the many subtypes of EDS, and general hypermobility, a categorization of all terms was created called the Hypermobility Spectrum Disorder. Patients present with...Read More
-

Blood Flow Restriction Therapy For The Treatment Of An ACL Reconstruction With A Meniscal Repair: A Case Report
Nicole Victor
ACL tears make up ~50% of all knee injuries. Meniscal tears are second to ACL injuries in regards to prevalence. Following an ACL reconstruction, high-load resistance training is often used to increase muscle strength. However, rehabilitation after a meniscal repair calls for a longer period of immobilization in order to prevent early loading of the meniscus. Blood Flow Restriction Therapy...Read More
-

Muscle Energy Techniques As Part Of A Comprehensive Plan Of Care For A Patient With Hip And Knee Osteoarthritis: A Case Report
Daniel White
Osteoarthritis (OA) is a chronic musculoskeletal condition which affects over 27 million Americans. The hip and knee joints are most affected by OA. Many risk factors are modifiable in the development of OA. While muscle energy techniques (MET) are commonly used to treat lumbopelvic dysfunction, limited evidence exists for its use as part of a comprehensive plan of care in...Read More
-

Functional Mobility In A Patient With Antiphospholipid Antibody Syndrome Following A Femoral Neck Fracture Surgical Repair: A Case Report
McKenna Young
Antiphospholipid Antibody Syndrome is an autoimmune disease which causes the body to produce antibodies that attack phospholipids, a type of fat. It leads to high rates of blood clot formation in arteries and veins. High rates of blood clots cause stroke, which can lead to balance concerns and increased falls. Fall rates among individuals with chronic disease peak between age...Read More
-

Delayed ACL Rehabilitation After Autograft Tear During Surgery: A Case Report
Rolene Yousefyan
Anterior cruciate ligament (ACL) injuries are one of the most common knee injuries in female soccer players that require reconstruction and rehabilitation. The incidence rate of autogenous ACL reconstruction (ACLR) complications during surgery are reported as low as 0.2% to 1.7%. There is insufficient information on the most effective rehabilitation protocol for patients with complications during surgery. Many rehabilitation protocols...Read More
-
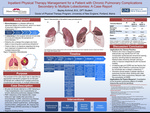
Inpatient Physical Therapy Management For A Patient With Chronic Pulmonary Complications Secondary To Multiple Lobectomies: A Case Report
Bayley Archinal
Bronchiectasis is a disease defined by abnormal dilation of the bronchi, which is a result of recurrent infections and/or chronic inflammation. A lobectomy is the surgical removal of one lobe of a lung and reduces the symptoms of bronchiectasis. Patients who undergo this surgery are more likely to have long-term pulmonary limitations. There is little to no literature regarding the...Read More
-

A Weighted Vest Rehabilitation Protocol To Improve Gait In A Patient With Cerebellar Degeneration: A Case Report
Amy Belanger and Kirsten Buchanan
The purpose of this case report was to investigate a combined weighted vest protocol and comprehensive PT program for a 34-year-old with cerebellar degeneration. Cerebellar degeneration (CD) is a rare brain dysfunction that affects motor control. Ataxia is a common manifestation of CD, defined as the discoordination of the limbs or trunk. Interventions that have separately been found to be...Read More
-

Intra-Rater & Inter-Rater Reliability In 2nd Year DPT Students Performing The Navicular Drop Test
Kirsten Buchanan, Nick Allard, David Buchan, Mike Curtin, and Andrew DiPartolo
The Navicular Drop Test (NDT) is used as a clinical measure of mid-foot pronation. Objective measurements are rooted in the trust of the tool. When utilizing the NDT, the tool is the practicing clinician. Research has revealed that experienced clinicians have good-excellent intra- and inter-rater reliability when measuring navicular drop (ND). Current data reports ~25,000 practicing US PTs have <...Read More
-
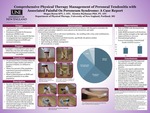
Comprehensive Physical Therapy Management Of Peroneal Tendonitis With Associated Painful Os Peroneum Syndrome: A Case Report
Megan Burns and Kirsten Buchanan
Treatment for peroneal tendonitis is well documented. Treatment of Painful Os Peroneum Sydrome (POPS) is not. Currently, there is no research that has investigated the best treatment for a combined diagnosis of POPS and peroneal tendonitis. The purpose of this case report was to investigate a comprehensive plan of care (POC) for a 65-year-old woman with a combined diagnosis of...Read More
-

The Treatment Of Pes Anserine Syndrome Using ACL Injury Prevention Exercises: A Case Report
Stephanie Chau and Kirsten Buchanan
The purpose of this case report was to utilize ACL injury prevention exercises within a comprehensive physical therapy (PT) plan of care (POC) for a patient with Pes anserine syndrome (PAS). Pes anserine syndrome (PAS) is the inflammation of either the pes anserine bursa, tendon, or both. The incidence and etiology of PAS are unknown at this time. There is...Read More
-

Comprehensive Physical Therapy Management Of A Patient With Decreased Shoulder Function And A History Of Breast, Lung, And Oral Cancer: A Case Report
Andrew Chongaway and Amy J. Litterini
Multiple primary cancers are uncommon in the same individual with an incidence rate of 2-17%. Surgery, chemotherapy, endocrine therapy, and Surgery, chemotherapy, endocrine therapy, and radiation may result in immediate and/or long radiation may result in immediate and/or long-term effects on the musculoskeletal, cardiopulmonary, nervous, and integumentary systems potentially resulting in decreased functional mobility and quality of life (QOL) for...Read More
-

Acute Care Physical Therapy And Early Mobilization For A Patient Following Bilateral Staged Anterolateral Total Hip Arthroplasties: A Case Report
Rachel Claussen
The purpose of this case report was to add to the limited literature describing acute care physical therapy (PT) management of patients receiving staged BTHA and to document both episodes of care. Primary hip osteoarthritis (OA) is a leading cause of significant hip pain resulting in disability, joint stiffness, and loss of function. 42% of people with hip OA have...Read More
-

Functional Mobility For A Patient With Myelodysplastic Syndrome, Chronic GVHD, And Corticosteroid Use: A Case Report
Alyssa Deardorff and Amy J. Litterini
The purpose of this case report is to describe PT interventions for an individual with a cancer diagnosis who received an allo-SCT and subsequently had long-term complications associated with cGVHD, long-term corticosteroid use, and cancer survivorship. Myelodysplastic Syndrome (MDS) is often called pre-leukemia as 1 in 3 individuals will develop Acute Myeloid Leukemia. It is a type of cancer that...Read More
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.