-

What Predicts Balance Exercise Intensity?
Margaret E. Chang, Vincente C. DeBack, Loren A. Klein, Eliana T. Madwed, Mikayla M. Matos, and Sophia L. Oliver
While it is known that exercise should be prescribed at a moderate to high intensity, the intensity of balance exercise that is actually prescribed during physical therapy isn't known. During this research project, student researchers completed observations of physical therapy sessions over 3 years. Linear regression analysis and correlational analysis was then used to investigate possible relationships between intensity of...Read More
-

Investigating Dual Task Balance Exercises: Quantifying Practice Patterns And Understanding Decision-Making Among Physical Therapists
Amelia Sabin, Wes Spagnuolo, Narissa Libby, and Kylie Berry
Dual-task exercise has been shown to be an effective intervention to improve patient functional outcomes and decrease falls. However, little is known about whether physical therapists are prescribing dual task exercises during their sessions, or at what intensity. The objective of this research was to analyze differences and similarities of observed balance exercise practice patterns and reported practice and decision-making...Read More
-

The Rehabilitation Of A 75-Year-Old Male Presenting With A Right Hip Flexor Strain Concomitant With Numerous Psychosocial Factors: A Case Report
Jillian Battista, Megan Chapski, Suma Varanasi, Jillian Witwicki, and Tara Paradie
Musculoskeletal disorders, often well understood, are a leading cause of disability worldwide. Concomitant psychosocial factors add a layer of complexity to the physical therapy treatment of musculoskeletal disorders. The purpose of this case report is to highlight the potential impact psychological factors have in the rehabilitation of musculoskeletal disorders, specifically the rehabilitation of a right hip flexor strain.
...Read More -

Development Of A Comprehensive Web-Based Prehabilitation Program For Gastrointestinal Cancer Survivors
Eric Norman, Maryam Nahidian, Amy J. Litterini, and Timothy Fitzgerald
Background: Individuals with frailty who undergo surgical procedures for gastrointestinal cancers are more likely to experience post-surgical complications, have a higher readmission rate, are more likely to be discharged to skilled care, and have an over four-fold risk of mortality. Developing targeted patient education tools and resources may support, and reduce complications for, individuals with frailty undergoing and recovering from...Read More
-

Physical Therapy Management Of Low Back Pain In A Young Female With Ankylosing Spondylitis Associated With HLA-B27 Antigen: A Case Report
Jake Adkins
Ankylosing spondylitis (AS) is a form of arthritis characterized by chronic inflammation of the axial skeletal system that causes back pain and loss of mobility with strong potential for slow, eventual spinal fusion. It affects 0.2-0.5% of the United States population and has no known cure, yet greater than 60 genetic components are involved. HLA-B27 is a genetic component highly...Read More
-

Return To Golf In A 71-Year-Old Female After A Mako Robotic-Arm-Assisted Unicompartmental Knee Arthroplasty: A Case Report
Katelyn Austin
Knee osteoarthritis (OA) is the most common joint disorder in the elderly. Unicompartmental knee arthroplasties (UKA) have been increasing in prevalence at a rate of 30% each year. Robotic-arm-assisted UKAs increases the accuracy of implant positioning compared to traditional techniques which helps with a quicker recovery. Little literature on UKAs, but total knee arthroplasty (TKA) interventions should focus on knee...Read More
-

Physical Therapy Interventions To Increase Independence With Functional Mobility For An Older Individual With Spinal Stenosis: A Case Report
Eleni Bautz
Spinal stenosis includes narrowing of the spinal canal which can affect nerves and other structures that pass through. Symptoms commonly associated with spinal stenosis are pain and paresthesia into the lower extremities. Spinal stenosis is diagnosed through patient history, clinical findings, and/or physical tests. Literature supports the use of physical therapy (PT) for conservative treatment in decreasing signs and symptoms...Read More
-

Rehabilitation And Prosthetic Training For An Individual With Bilateral Lower Extremity Amputations Due To Peripheral Vascular Disease: A Case Report
Morgan Bessette
Peripheral vascular disease (PVD) is a condition in which there is a disruption of blood flow to the extremities. Common causes of PVD include: hypertension (HTN), smoking, cardiac disease and/or diabetes. 12 to 20% of the population greater than 60 years old are affected by PVD. PVD can cause intermittent claudication or critical limb ischemia (CLI) and is therefore the...Read More
-

Effects Of Sleep Hygiene In The Hospital
Tina Bhakta, Paxton Arsenault, Maya Ahluwalia, and Rachel Coats
Research poster by UNE Occupational Therapy and Physical Therapy students investigating the definition of and recommendations for good sleep hygiene, the limitations of the hospital setting on attainment of sleep hygiene, and the benefits of sleep hygiene for hospital patients.
... Read More
-

Regaining Independence In Ambulation For A Visually Impaired Patient With Rhabdomyolysis: A Case Report
Brandon Bourgoin
Rhabdomyolysis is a myopathic condition with an acute onset that causes a rapid degradation of muscle tissue. It causes a significantly elevated release of creatine kinase (CK), a muscle enzyme that is a cellular component in healthy muscle tissue, into the blood stream. Common causes include muscle trauma (injury/strenuous activity), drug/alcohol abuse, medications, toxins, infections, and extended periods of immobility....Read More
-

Differences In Mechanics Between First And Second Drop Vertical Jump Landings
Kirsten Buchanan, Irene S. Davis, Devin A. Finnegan, Brooke I. Flaherty, Jordan G. Lamb, Elisabeth M. Michaud, and Bryan J.M. Raksnis
A drop jump and landing, followed by another maximal jump and landing, has been used when assessing injury risk utilizing the Landing Error Scoring System (LESS). Vertical ground reaction force (vGRF) and knee excursion are also commonly analyzed during a drop vertical jump. Previous studies have assessed initial drop vertical jump landing mechanics without assessing the second landing from the...Read More
-

Physical Therapy Intervention For An Elderly Patient With Comorbidities Following Surgical Fixation Of A Femoral Neck Fracture: A Case Report
Yu-min Chou
More than 300,000 elderly people over age 65 required hospitalization due to hip fracture in 2016. More than 95% of hip fractures are the result of falls. Strength training programs are suggested for geriatric patients with surgical fixation following hip fracture. Returning to prior level of function and quality of life is the primary goal of rehabilitation for geriatric patients...Read More
-

Interdisciplinary Administration Of LSVT-BIG By A Physical Therapist And Occupational Therapist On A Patient With Parkinsonism: A Case Report
Shelby Clare
The clinical diagnosis of parkinsonism is “the presence of at least two of the four cardinal signs: resting tremor, rigidity, bradykinesia, and postural instability.” Symptoms often lead to limited functional mobility. Patients who have unilateral bradykinesia with hypokinesia, changes in gait, balance, and decreased quality of life have positively responded to Lee Silverman Voice Technique (LSVT) BIG treatment according to...Read More
-

Acute Inpatient Rehabilitation Of A Patient Following A Pontine Stroke With Limited Recorded Medical History: A Case Report
Russell Curl
795,000 strokes occur annually in the United States, or one every 4 seconds. Impairments following a stroke may include deficits in strength, coordination, sensation, and language skills. Expected impairments of pontine strokes include hemiplegia, sensorimotor dysfunction, ataxic hemiparesis, and dysarthria. There is little current research on pontine strokes. The purpose of this case report is to outline the physical therapy...Read More
-

Functional Mobility Interventions For A Bariatric Patient With Necrotizing Fasciitis: A Case Report
Jakub Cwalinski
Necrotizing Fasciitis is a life threatening soft tissue infection that is characterized by a rapid spreading infection of the subcutaneous tissue. Symptoms include red or purple skin in the affected area, severe pain, fever, and vomiting. Typically, the infection enters the body through a break in the skin such as a cut or burn. Surgical debridement is the mainstay of...Read More
-
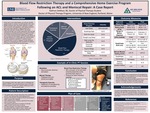
Blood Flow Restriction Therapy And A Comprehensive Home Exercise Program Following An ACL And Meniscal Repair: A Case Report
Kathryn DeMoor
Every year in the United States, up to 60 per 100,000 people sustain an anterior cruciate ligament (ACL) tear. Medial meniscus tears have been reported in roughly 60% of the ACL tear population, while lateral meniscus tears have been reported in approximately 30%. Blood flow restriction therapy (BFRT) has shown improved strength and muscle hypertrophy with low load exercises by...Read More
-

Conservative Management Of A Massive Rotator Cuff Tear And Partial Tear Of The Long Head Of The Biceps: A Case Report
Jessica Diggins
A rotator cuff tear (RCT) is a common injury to the shoulder musculature that increases in prevalence with age. RCT’s can be classified into five categories determined by the muscular involved: Type A: supraspinatus & superior subscapularis; Type B: supraspinatus & entire subscapularis; Type C: supraspinatus, superior subscapularis & infraspinatus; Type D: supraspinatus & infraspinatus tears; Type E: supraspinatus,infraspinatus &...Read More
-

Oncologic And Orthopedic Rehabilitation For A Pancreatic Cancer Survivor Following Total Knee Arthroplasty Revision: A Case Report
Kelsey Dumond and Amy J. Litterini
An estimated 80% of cancer survivors undergoing chemotherapy or radiation to manage their cancer will experience cancer-related fatigue (CRF). The majority of cancer survivors are elderly – a population frequently affected by osteoarthritis (OA). Physical activity is the most recommended and evidence-based non-pharmacologic intervention for CRF. Strong evidence exists for lower-extremity resistance and functional exercise following Total Knee Arthroplasty (TKA)....Read More
-

Gait, Strength, And Balance Training For A 43-Year-Old Male Following Acute Right Middle Cerebral Artery Stroke: A Case Report
Victoria Dwyer
A cerebrovascular accident, commonly known as a stroke, is caused by an ischemic or hemorrhagic event affecting arteries that lead to the brain causing them to burst or be occluded. The middle cerebral artery is the most commonly occluded artery involved in a stroke. The four most common risk factors involved in having a stroke are: high blood pressure, diabetes,...Read More
-

Treatment Approach For Traumatic Myositis Ossificans Using Ultrasound And Stretch Protocol: A Case Report
Paul Eo
Traumatic Myositis Ossificans (MO) can happen at any age, but the highest prevalence occurs in young active males after trauma (60-75% are traumatic). MO can occur from repetitive minor trauma, which is common in horseback riders who develop MO in the adductors and shooters who present with MO in their deltoid. Patients with MO commonly present in the clinic with...Read More
-

Functional School-Based Physical Therapy Management For A Child With Pallister-Killian Syndrome: A Case Report
Cheryl R. Espinosa and Molly Collin
Pallister-Killian Syndrome (PKS) is a rare genetic disorder caused by an additional short arm in chromosome 12. PKS affects multiple systems, which can impact a child’s development. Common clinical manifestations include: hypotonia, visual impairment, hearing loss, coarse facial features, intellectual disability, and congenital heart defects. Improvements in gross motor function have resulted from physical therapy (PT) and rehabilitation involving neurodevelopmental...Read More
-
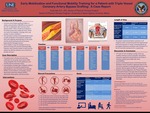
Early Mobilization And Functional Mobility Training For A Patient With Triple Vessel Coronary Artery Bypass Grafting: A Case Report
Cody Hall
Coronary artery bypass grafting (CABG) is a widely used procedure (200,000 annual cases in the US)1 in individuals with Coronary artery disease (CAD). CAD is a build-up of plaque in the blood vessels that supply the heart, which can result from diabetes, smoking, and a vast number of other conditions. The procedure involves harvesting blood vessels (usually autografts of the...Read More
-
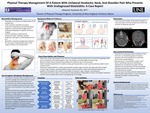
Physical Therapy Management Of A Patient With Unilateral Headache, Neck, And Shoulder Pain Who Presents With Undiagnosed Mastoiditis: A Case Report
Alexandr Kostenko
Mastoiditis is an infection and inflammation of the mastoid cells. If left untreated, mastoiditis can lead to intracranial complications and ultimately death. Diagnosis is confirmed with imaging such as computed tomography or magnetic resonance imaging. Common symptoms include earache, retroauricular pain, headache, mastoid tenderness, hearing loss, and discharge from the ear. Mastoiditis is typically managed with antibiotics, but may require...Read More
-

Comprehensive Physical Therapy Management Of Chronic Low Back Pain With Associated Remote Right Hamstring Injury: A Case Report
Emily Larson
Low back pain (LBP) is a health condition associated with back, core, and hip muscle dysfunction as well as reduced lumbar range of motion. Core muscle stabilization, hip abductor strengthening, and lumbar range of motion are all effective techniques for treating patients with chronic LBP. Lumbar muscular imbalance can lead to hamstring injury because of change in the functional load....Read More
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.



